say: meth-oh-TREX-ate

POG protocols for ALL traditionally include IV methotrexate as the backbone of the therapy; CCG protocols developed using BFM therapy. On POG protocols, methotrexate used to require an in-patient stay for a 24 hour infusion; some current protocols (2004) are testing to see if a 4 hour out-patient administration of methotrexate is feasible. Not all CCG protocols employ IV methotrexate, instead, it is administered orally and in spinals. See also "Notes on Doses of Methotrexate" (below).
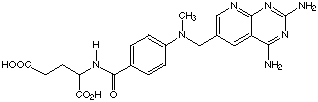
The CA name for methotrexate is: N[4-[[(2,4-diamino-6-pteridinyl)methyl]methylamino]benzoyl]-L-glutamic acid. The CA registry number is 59-05-2. Common synonyms: Mexate, Methylaminopterin, Emtexate, Metatrexan, Methopterin, MTX dihydrate, Folex, Folex PFS, Amethopetrin. Methotrexate is an antineoplastic, an antirheumatic, a nucleic acid anti-metabolite (like 6-MP,above), and a "folic acid antagonist".
Hmm, folic acid, a necessary nutrient. Let's see, I have a structure of folic acid on my hard drive, let's compare:
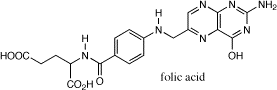
You can see that the nitrogen group has a CH3 on it and there is an OH group on the double ring instead of an NH2 group. Enough to make a difference in a biosynthesis scheme!
At two stages in the biosynthesis of purines (adenine and guanine) and at one stage in the synthesis of pyrimidines (thymine, cytosine, and uracil), one-carbon transfer reactions occur that require specific coenzymes. These coenzymes are synthesized in the cell from tetrahydrofolic acid. Tetrahydrofolic acid itself is synthesized in the cell from folic acid with the help of an enzyme, folic acid reductase. Methotrexate looks a lot like folic acid to the enzyme, so it binds to it thinking that it is folic acid. In fact, methotrexate looks so good to the enzyme that it binds to it quite strongly. All the folic acid reductase enzymes in the cell bind merrily to the methotrexate and ignore any folic acid they might see. Thus, DNA synthesis cannot proceed because the coenzymes needed for one-carbon transfer reactions are not produced from tetrahydrofolic acid because there is no tetrahydrofolic acid. Again, without DNA, no cell division.
Most of the parents of cancer kids have been told not to give folic acid supplements during chemo since it interferes with the action of the methotrexate.
Methotrexate has a general toxicity because it affects all rapidly dividing cells, such as those in the intestinal mucosa and prevents the production of tetrahydrofolate from folic acid in all tissues. Tetrahydrofolate is a necessary compound in many biosynthetic pathways, not just the synthesis of DNA. One of these is the synthesis of L-glutamate. One parent told us that her oncodoc recommended glutamic acid supplements, and that they helped her child immensely. Makes sense.
Methotrexate can be given either by mouth, IV, intramuscular, or intrathecally (spinal fluid). It is yellow in color.
Notes on Dosages of Methotrexate: IV ID (intermediate dose) methotrexate is1g/m2, HD (high dose) is 2.5g/m2, as given IV over 4-24 hours, usually with leukovorin rescue. CCG protocols that include "escalating" IV methotrexate administer it 0.10 g/m2 over 10-15 min, then escalate each subsequent dose by 50mg/m2/dose to toxicity. When given PO, methotrexate is 15-20 mg/m2/day in maintenance. POG employs 4 PO doses of mtx, each 25mg/m2, for 100mg/m2/day in intensive continuation.
Common side effects listed by our hospital (and this :probably means they do not have to be reported to the docs, except my sheet says to call the doc if mouth sores develop)
Less common side effects:
(All of the adverse effects reverse when the drug is discontinued.)
Also listed by the hospital: the possible adverse effects of this drug are mouth lesions in the form of painful patches on the lips, gums and mucosa of the mouth. These clear rapidly with stopping the drug. Along with mouth ulcers, there can also occur ulceration of other parts of the digestive tract with abdominal pain, vomiting and diarrhea. This drug can depress the bone marrow, which leads to a depression of white blood cells, platelets, and red blood cells.
This means that they will be monitoring your CBC. With high doses of methotrexate, they will monitor fluid intake and urine output closely. Leucovorin is a medicine that may be prescribed. Leucovorin is an antianemic and an antidote for folic acid antagonists. Leucovorin is the active form of the B complex vitamin, folate. Another name for Leucovorin is folinic acid: the very name I found in a biochem text - it said that it could help alleviate the effects of methotrexate! "Leucovorin is used as an antidote to drugs that decrease levels of folic acid. Folic acid helps red and white blood cell formulation and the synthesis of hemoglobin. Some treatments require what is called leucovorin rescue, because the drug used to treat the cancer or other infection has had an adverse effect on folic acid levels. Leucovorin is used to reduce anemia in people taking dapsone, a preventive treatment for PCP. Leucovorin is also used in combination with chemotherapy such as methotrexate." (The words in "" are from the link on Leucovorin given above.)
Certain medicines will increase methotrexate side effects and may not be taken before, during, or shortly after receiving methotrexate. These drugs include:
To stave off the ill effects, drink at least 2 quarts of high calorie fluids such as juices and nectars per day. If treatment is in pill form, take 1 hour before or 2 hours after meals. Report any unusual bleeding to your doctor. Use a soft toothbrush and electric razor. Do not drink alcoholic beverages or take drugs containing aspirin. Avoid use of over-the-counter drugs without first consulting with your doctor or pharmacist.